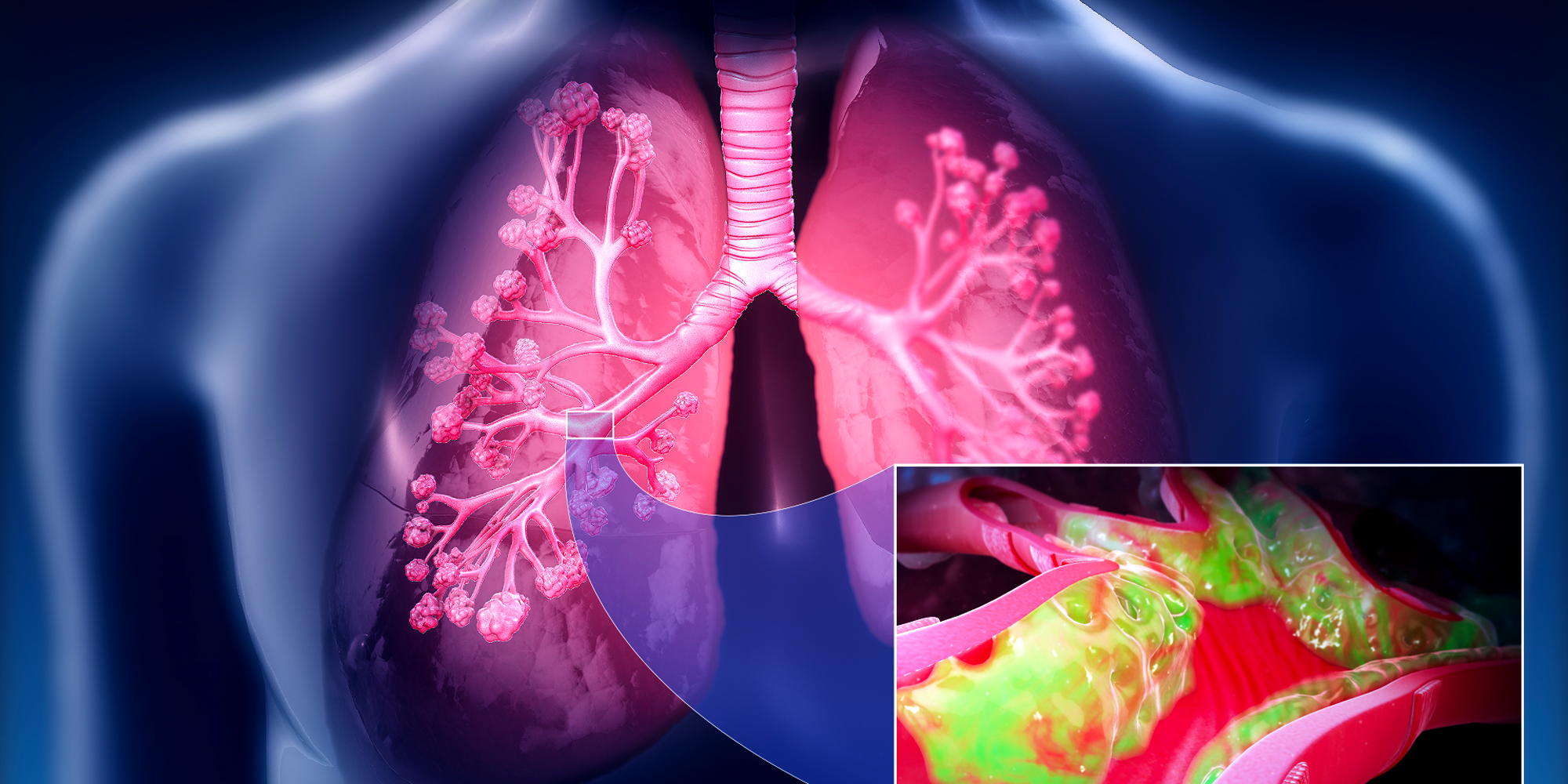
Chronic obstructive pulmonary disease (COPD) is a huge global health problem; it is the third most common cause of death worldwide. The number of patients in Poland exceeds two million, with approximately 20% of patients having the advanced form of the disease, characterized by chronic cough and shortness of breath on exertion. Smog, tobacco smoke and occupational exposure to harmful dust are the main causes of COPD.
One of the early symptoms of the disease is cough. The patient may cough up a small amount of sputum, and the wet cough lasts most of the year and increases in the morning. In most cases patients ignore this symptom, for example by associating it with an inherent side effect of cigarette smoking.
COPD is diagnosed on the basis of biomedical history, spirometric measurement and additional examinations, which require a specialist medical visit and a number of tests that many people do not opt for quickly. Therefore, about two-thirds of patients miss the opportunity to be diagnosed with COPD at an earlier stage, and late diagnosis often leads to a rapid worsening of symptoms and progression of the disease.
In the project initiated by Recumed Sp. z o.o. and co-funded by the National Center for Research and Development, it is proposed to develop an innovative product for in vitro diagnosis of COPD in saliva, which will provide an easy and fast way to detect the disease and determine its stage. The final product will consist of an immunochemical test and a mobile application, and its potential users will be family doctors, pulmonologists and individuals.
Biomedical expert of the project (POIR.01.01.01-0610/20-00), Dr. Magdalena Rudzińska-Radecka, together with her team is conducting research to assess the levels of selected biomarkers (C-reactive protein- CRP, procalcitonin – PCT, neutrophil elastase – NE and antitrypsin – AAT) in the saliva of patients with COPD.
The project’s first phase is to determine the correlation between saliva and blood serum concentrations (determined by immunoenzymatic ELISA assay) of the indicated biomarkers in 70 healthy volunteers, validating that saliva can be a proper diagnostic medium. This is an essential part of testing for rapid diagnosis, as saliva collection is non-invasive and does not require complex laboratory techniques and proper transport, unlike blood.
For Phase 2, the team plans to conduct molecular testing of saliva from healthy (70 smokers, 70 non-smokers) and COPD volunteers (70 smokers, 70 non-smokers at various stages of disease progression), along with spirometry testing and medical history collection from all volunteers. These data will serve as reference values for both the biosensor prototype under development and for machine learning.
It is expected that the developed sensor will qualitatively and quantitatively indicate the levels of the tested markers with high accuracy compared to the reference ELISA method. The biosensor will operate using lateral flow assay technology, with a drop of saliva moving along a nitrocellulose membrane on which specific antibodies in complex with colloidal gold will be immobilized. After the sample has been absorbed by the membrane, the antigen (if positive) will bind to the localized gold-antibody complex, resulting in a color reaction of varying intensity. The test will be placed in the 3D printed platform.
Machine learning specialist Robert Marczyński says that machine learning technologies are applicable in all areas of daily life, including healthcare. Based on the experimental data, a computer can make autonomous decisions without programming it for specific tasks. Thus, using the biomedical data from different groups (the control group and the study groups), we can teach the machine to recognize and correlate the factors with disease and its progression.
In this context, the result of the third phase of the project will be the development of a set of self-learning algorithms that will appropriately correlate the level of the biomarkers in saliva, spirometry measurement values and clinical information about volunteers. Eventually, it will be a base for a machine how to identify the disease and its severity. All of this will be developed as a mobile application.
Finally, the result obtained from the biosensor will be able to be easily and quickly interpreted using each user’s own phone.
The produced prototype of the target set will be further developed into a version in which the developed technology will be confirmed in real conditions.
It is hoped that the research undertaken by the team will help to accelerate the diagnosis of COPD and thus save the lives of many patients.
For more information on the research conducted by Dr. Magdalena Rudzińska-Radecka, please check:
https://www.linkedin.com/in/magdalena-radecka-rudzi%C5%84ska-9891345a/
https://sgmte.pl/team/magdalena-radecka/
https://orcid.org/0000-0001-9912-2128
Natalia Mikulska